Updated May 21, 2020. Changes in Red
There’s been a flurry of posts and questions on this site about COVID-19, the Trump administration’s response to the crisis, and what to do if cases start being reported in your area. While I don’t work directly with medical care or this family of viruses, I have a PhD in Immunology. For whatever that’s worth, I would like to offer this post as either a place where you can ask questions about the disease or talk about your fears and frustrations.
- How dangerous is COVID-19 on an individual level?


As you can see, it is mainly dangerous to the elderly and those with underlying health conditions. But younger people can still get sick and die.
2. What about children and pregnant mothers?
COVID-19 appears to affect children less often, and with less severity, including frequent asymptomatic or subclinical infection. There is evidence of critical illness, but it is rare. The role of children in transmission is unclear, but consistent evidence is demonstrating a lower likelihood of acquiring infection, and lower rates of children bringing infections into households. Changes in laboratory or radiographic parameters are slightly different to adults, and changes usually mild. There is some evidence of vertical transmission to neonates, however it is unclear is this is perinatal or intrauterine. Evidence suggests both infected mothers and infants are no more severely affected than other groups. There does not appear to be significant increased risk for children with immunosuppression, but further data is needed. Children with respiratory and complex neurodisability appear more likely to suffer complications, however not obviously more than would be expected from infection with other respiratory viruses. May 15 conclusion by Don’t Forget The Bubbles, a site that collates paediatric literature of Covid-19
Multisystem Inflammatory Syndrome in children and adolescents temporally related to COVID-19. It is expected to be rare and treatable.
3. How does it spread?
The disease can spread from person to person through small droplets from the nose or mouth which are spread when a person with COVID-19 coughs or exhales. These droplets land on objects and surfaces around the person. Other people then catch COVID-19 by touching these objects or surfaces, then touching their eyes, nose or mouth. People can also catch COVID-19 if they breathe in droplets from a person with COVID-19 who coughs out or exhales droplets. This is why it is important to stay more than 1 meter away from a person who is sick. Source:WHO.
ETA May 22: CDC has revised its guidelines on COVID-19 spread. It puts a greater emphasis on person to person spread, and less emphasis on fomite spread.
Being outdoors is safer when it comes to transmission (one preprint estimates 18.7X safer) but not foolproof. The COVID-19 settings of transmission – database has now collated multiple incidences of transmissions in outdoor settings so please keep 6 feet apart with people who are not members of your household, even when outdoors.
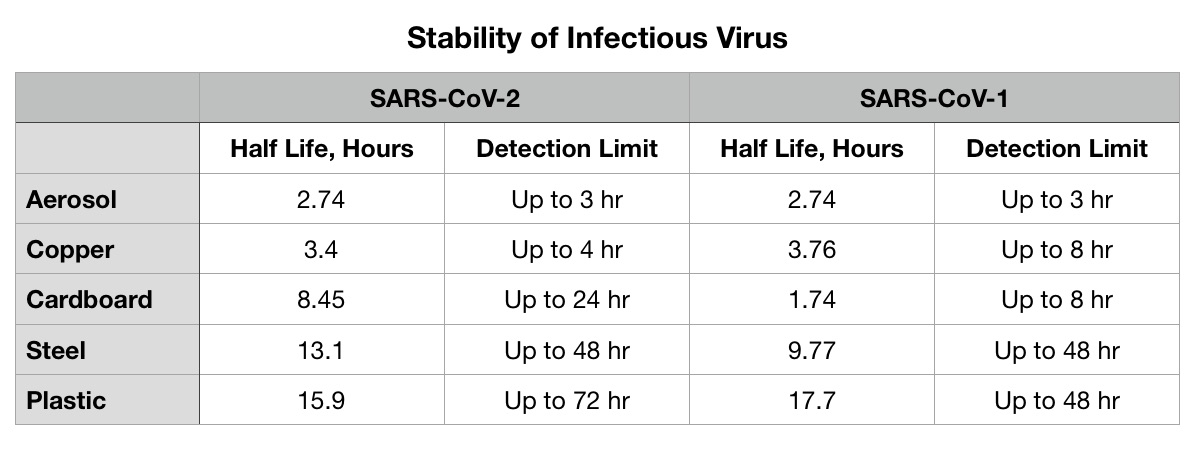

Surfaces can be efficiently inactivated by surface disinfection procedures with 62–71% ethanol, 0.5% hydrogen peroxide or 0.1% sodium hypochlorite within 1 minute.
4. What are the symptoms?


Covid-19 Symptom Checker Tool by CDC and Emory University
5. Asymptomatic and presymptomatic spread
Percentage of transmission occurring prior to symptom onset is 40%. Source: CDC
14 patients (1.4%) remained true asymptomatic in a large Chinese study. Source: NUS Literature Roundup
6. What is the incubation period?
Most estimates of the incubation period for COVID-19 range from 1-14 days, most commonly around five days. Virus shedding can occur in the 24-48 hours prior to symptom onset. Source: WHO

7. Do masks work to prevent spread of disease?
If you’re already sick and coughing, it acts as a barrier to prevent cough droplets from travelling far. If you’re healthy, you’re more likely to pick up the virus by touching a surface that an infectious droplet landed on. Given there’s a global shortage of masks and counterfeit masks flooding the market, it’s recommended that you only use masks if you are sick or caring for a sick person.
If you must use a mask, learn how to use it properly at this WHO page. In particular, if you touch the front of the mask while it’s still on, any contamination on it can be introduced into your mouth, which defeats the purpose.
ETA Apr 16 2020: CDC recommends cloth masks for general public to wear to prevent presymptomatic transmission. NYT article on ways to make your own cloth masks.
8. What should I do to avoid getting infected or spreading the disease?
List summarized from WHO guidelines.
- Regularly and thoroughly clean your hands with an alcohol-based hand rub or wash them with soap and water.
- Maintain at least 1 metre (3 feet) distance between yourself and others.
- Avoid going to crowded places.
- Avoid touching eyes, nose and mouth.
- Cover your mouth and nose with your bent elbow or tissue when you cough or sneeze. Then dispose of the used tissue immediately.
- Stay home and self-isolate even with minor symptoms such as cough, headache, mild fever, until you recover. Have someone bring you supplies. If you need to leave your house, wear a mask to avoid infecting others.
- If you have a fever, cough and difficulty breathing, seek medical attention and call in advance. Do not show up at a clinic or hospital unannounced. Follow the directions of your local health authority.
- Keep up to date on the latest COVID-19 hotspots (cities or local areas where COVID-19 is spreading widely). If possible, avoid traveling to these places – especially if you are an older person or have diabetes, heart or lung disease.
- Clean high touch surfaces (e.g. phones, laptops) regularly.
9. How worried should I be?
Estimated R0 for SARS-CoV-2 is 5.7. This means >82% of the population has to be immune, through either vaccination or prior infection, to achieve herd immunity to stop transmission. Otherwise, population contact reduction must go down between 25 to 50% to contain transmission. Source: Los Alamos National Laboratory
COVID-19 Projections is outdoing the ensemble projections by the CDC.
10. Flattening the curve to reduce the burden on the healthcare system

Further reading: Coronavirus: Why You Must Act Now by Tomas Pueyo, Flatten The Curve Guide, UCSF Expert Panel Predictions
11. How do I prepare for an outbreak in my area?
These are the two problems that will likely affect you even if you are lucky to remain uninfected. The healthcare infrastructure will be overstretched and people will panic buy and hoard much more than they need. If you can avoid either, you’ll help to keep the problem from getting worse.
To avoid having to go to the clinic/hospital: A thermometer, some masks for if you start coughing, fill your prescriptions and get basic medications to tide you through not having to go to clinics or pharmacies. If you get a fever and a cough, call a doctor first before using something that would mask the symptoms so you can report symptoms accurately.
To avoid panic buying: Enough non perishable food to last 2-3 weeks quarantine. Do it a bit at a time, not all at once. When you are done, stop. Hand sanitizer is convenient but if you run out, don’t panic because water and soap is all you need.
Here’s two handy guides on how to prepare. Scientific American article. One-page checklist.
12. How do I self quarantine or care for a sick housemate?
There is a very real possibility that if the healthcare infrastructure becomes overtaxed, that you will have to stay at home through the duration of your illness and/or have to care for someone else. The goal here is isolation of the quarantined/infected person away from communal spaces in the dwelling.
Prepare a room, preferably with a personal bathroom. If the infected person has mild symptoms, you can leave everything they would need outside their door for pickup, e.g. food, medicine, disinfectant for surfaces, clean clothes, personal hygiene products, entertainment devices, communication device, a thermometer and some means to keep record of symptoms, etc. Don’t share any items.
As caregiver, if you have to enter the room, protect yourself from aerosols and contact with soiled items. E.g. masks, gloves (or substitute with plastic bags), etc. Wash your hands frequently. And you will be stuck with getting supplies and keeping the rest of the dwelling clean.
If only a shared bathroom is available or the infectee must enter common areas, clean common surfaces, laundry and dishes safely. The infectee should wear a mask in trips to the shared bathroom or common areas. See MIT Q&A for more details.
Further reading: How to Self Quarantine, CDC guide on environmental cleaning and disinfection
13. I think I have COVID-19 symptoms but won’t be able to get tested.
If you live in the US, Canada, or Mexico, you can report current symptoms to COVID Near You, a resource run by Harvard Medical School that is an offshoot of their Flu Near You project. Please read FAQ page here. Identifying data will not be collected.
14. That “coronavirus is a bioweapon” theory is bullshit right?
Indubitably. SARS-CoV-2 (the name given to the virus itself) achieved strong binding to the human ACE2 receptor by making a mutation that would not have been predicted by previous studies. That is to say, a scientist trying to weaponize a coronavirus based on prior knowledge would have picked a different mutation to use. Nor does SARS-CoV-2 look like it has any of the marks left by known genetic manipulation techniques.
Could a scientist have taken a wild SARS-CoV-2 virus, adapted it to infect humans using the virus’ natural propensity to mutate, and deliberately or accidentally released it? Unlikely. The human virus sequence is too similar to the bat sequence to have mutated for a long period of time in culture, but the acquisition of the polybasic cleavage site, according to influenza studies, requires intense culture, at which point the virus is likely to have mutated other parts as well.
Correspondence published in Nature. Blog post with description for laypeople.
15. One page summary primarily for doctors

16. What reliable resources, other than mainstream newspapers, can I use to keep myself informed?
- What You Can Do About Coronavirus Right Now by the New York Times is the most extensive and high signal-to-noise summary of what you can do to prepare and care for a sick household member.
- World Health Organization
- UpToDate is the database used by doctors to summarize the latest findings. It has a “for patients” section with lay person explanations.
- This Week in Virology is a podcast by 4 virologists who discuss the latest findings and answer questions.
- Coronavirus Global Cases dashboard by Johns Hopkins University. I prefer changing the display to existing cases instead of cumulative cases.
- Financial Times has a great regularly updated page of graphs
- Our World In Data and 91-DIVOC are excellent for exploring and visualizing latest data
- List of Twitter scientists that are good follows
- Weekly scientific literature roundup from Emory University and National University of Singapore. The NUS summary is more lay person friendly.
17. Other resources
Coronavirus Relief Resource page that covers city, state and federal relief for those impacted economically by Covid-19 and isn’t all about NY.
- Confused about different state’s actions and quarantine orders? See Covid-19 Action Tracker to quickly find out that information.
- Mental health coping strategies
- Working from home
- Parenting/home school discussion
- Sobracadoes – Remote AA meetings for quarantine
- Live arts streaming and how to support performing artists
- Borrowing ebooks using your library membership
- Audible has made a collection of audiobooks for children and teens free for listening without a membership
- How to avoid COVID-19 phishing scams and fake health advertising
- How to identify social media bots spreading misinformation about COVID-19
18. I want to help! How can I help?
Most volunteer work will be local so that’s a good starting point to look for ways to help.
- Help ensure food security for the vulnerable: old, immune suppressed, children, undocumented, etc by packing and distributing
- Blood donation has decreased dramatically so you can donate blood if you’re up to it.
- Hospitals are running out of personal protective equipment like gloves and masks. If you can sew, they will accept homemade face masks. A list of who to contact to donate personal protective equipment.
- Join Folding@Home to donate your computer’s processing power when it is sitting idle toward protein folding models for the Covid-19 effort. Avocado guide by Monsieur Glitch here.
- Financial donations are always welcome.
- Keep your local businesses alive by buying a gift card to be used at a later date.
Happy to take more suggestions.
19. What comes next? The sequel post is here.
Feel free to use this space to ask any questions and help each other out. Anyone who might know more than I do about this topic, please chime in.


You must be logged in to post a comment.